Why Is There Fluid in My Lungs? Common Causes of Pleural Effusion
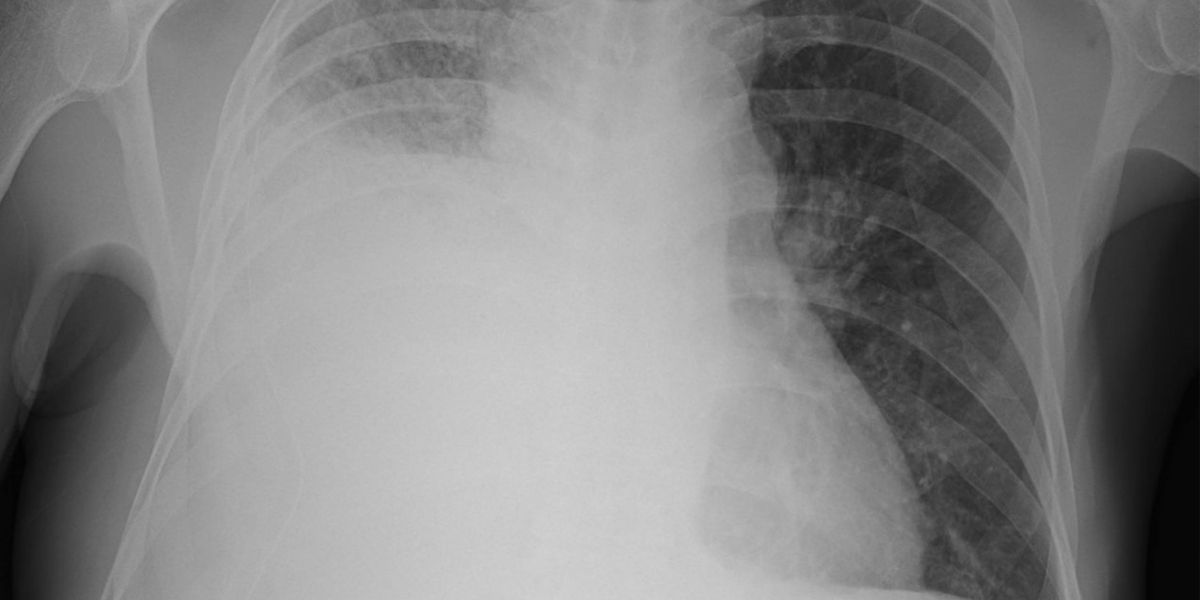
Fluid in the lungs can sound alarming, and for good reason. When breathing becomes uncomfortable or painful, and a persistent cough will not go away, many people begin to worry about what is happening inside their chest. One possible explanation is pleural effusion, a condition in which excess fluid collects in the space surrounding the lungs. While the lungs themselves are designed to expand and contract with each breath, they sit inside a thin lining called the pleura. Between these layers is a small amount of fluid that allows smooth movement during breathing. When too much fluid accumulates, it can interfere with normal lung function.
Pleural effusion is not a disease in itself. Instead, it is often a sign of another underlying medical problem. Understanding why this fluid builds up is the first step toward proper treatment. Some causes are mild and temporary, while others require urgent medical care. Knowing the most common reasons for pleural effusion can help you recognize symptoms early and seek appropriate evaluation.
What Is Pleural Effusion?
Pleural effusion occurs when excess fluid collects in the pleural space, the thin gap between the lungs and the chest wall. Under normal conditions, only a few teaspoons of fluid are present. This small amount acts as lubrication, preventing friction as the lungs expand.
When the balance between fluid production and drainage is disrupted, fluid begins to accumulate. As it increases, the lungs may not fully expand. This can lead to shortness of breath, chest discomfort, and decreased oxygen levels. Doctors often categorize pleural effusion into two main types: transudative and exudative. This distinction helps determine the underlying cause.
Congestive Heart Failure
One of the most common causes of pleural effusion is congestive heart failure. When the heart cannot pump blood effectively, pressure builds up in blood vessels. This increased pressure can force fluid out of the vessels and into surrounding tissues, including the pleural space.
In heart failure-related pleural effusion, the fluid is usually transudative, meaning it results from pressure changes rather than inflammation or infection. Patients may notice swelling in their legs, fatigue, and worsening shortness of breath, especially when lying flat. Treating the heart condition often reduces the fluid buildup.
Pneumonia and Lung Infections
Infections of the lungs, such as pneumonia, frequently lead to pleural effusion. In these cases, inflammation causes fluid to leak into the pleural space. This type of effusion is usually exudative, meaning it is associated with infection or inflammation.
When pleural effusion develops alongside pneumonia, it is sometimes called a parapneumonic effusion. Symptoms may include fever, chills, chest pain that worsens with deep breathing, and a productive cough. If the fluid becomes infected, it can turn into an empyema, a more serious condition that requires drainage and antibiotics.
Cancer-Related Pleural Effusion
Certain cancers can cause fluid to accumulate around the lungs. Lung cancer and breast cancer are among the most common causes, but lymphoma and other cancers may also be involved. Cancer-related pleural effusion typically occurs when malignant cells spread to the pleura, disrupting normal fluid balance.
Patients may experience progressive shortness of breath, weight loss, and a persistent cough. In some cases, pleural effusion is the first sign of an undiagnosed cancer. Doctors may analyze the fluid through a procedure called thoracentesis to check for cancer cells and guide further treatment.
Pulmonary Embolism
A pulmonary embolism, or blood clot in the lungs, can also lead to pleural effusion. When a clot blocks blood flow in the pulmonary arteries, it may cause inflammation and increased pressure in nearby vessels. This can result in fluid leaking into the pleural space.
Symptoms often include sudden chest pain, shortness of breath, rapid heart rate, and sometimes coughing up blood. A pulmonary embolism is a medical emergency and requires immediate attention. Imaging tests such as CT scans help confirm the diagnosis.
Liver and Kidney Disease
Chronic liver disease, particularly cirrhosis, may cause pleural effusion through a condition known as hepatic hydrothorax. In these cases, fluid from the abdomen moves into the chest cavity through small openings in the diaphragm.
Kidney disease can also contribute to fluid buildup when the body retains excess salt and water. Reduced kidney function may lead to generalized swelling, including in the pleural space. Managing the underlying liver or kidney condition is essential to controlling recurrent effusions.
Autoimmune and Inflammatory Conditions
Autoimmune disorders such as lupus and rheumatoid arthritis can cause inflammation of the pleura. This inflammation increases fluid production and may result in exudative pleural effusion.
Patients with autoimmune-related effusions may also experience joint pain, skin rashes, or other systemic symptoms. Identifying the underlying inflammatory condition allows doctors to tailor treatment with medications that control immune system activity.
Conclusion
Pleural effusion is a sign that something in the body requires attention. Whether the cause is heart failure, infection, cancer, blood clots, or chronic organ disease, fluid around the lungs should never be ignored. Early diagnosis significantly affects treatment options and overall outcomes. If you are experiencing unexplained shortness of breath, chest discomfort, or a persistent cough, a thorough medical evaluation is essential. The specialists at Prana Pulmonary Clinic can provide a comprehensive assessment and personalized care to identify the cause of pleural effusion and guide you toward appropriate treatment.